|
Two weeks ago I saw my orthognathic surgeon for a 6-month (actually 7-month) check on my recovery progress. We are both thankful he wanted to see me then, instead of waiting for a 1-year checkup. Within moments of feeling my maxilla, he told me we’ll have to do another surgery. The healing process is not going properly, and it requires surgical intervention. We scheduled the surgery for this Wednesday, April 12, 2017.
As you may recall, the outcome we were expecting/hoping for after the August 17, 2016 surgery was the “bony union” in my healing. What he believes he is seeing is “fibrous non-union of maxilla”. Another way of describing this is to say that my hard palate and upper teeth can move independently of the rest of my bony skull, because the cuts have not healed properly. So, for example, if I’m chewing on something, my hard palate flexes according to the pressure I put on it. The fact is, I’ve been aware of this phenomenon for months; it’s been continuous throughout my recovery. I did not know that it was not a normal part of the recovery. It had been gradually lessening, I thought, though my orthodontist had recently been concerned that it seemed more, not less, flexible. I wish that I had known this was something important to report to my surgeon. (He wishes it, too – while not blaming me for not reporting it.) This does connect to what I feel is a larger issue in American health care: the disconnect in communication between health care providers and their patients. I hasten to point out that my surgeon has gone out of his way to communicate with me; he’s called me at home several times for really valuable conversations, and has been entirely open to my questions and thoughts in our appointments. But, I think there is a systemic discouragement (or, put more accurately, lack of encouragement) of patients asking questions and being in touch with their doctors. This is much more of a topic than I can address now – but it’s absolutely something I’ll be raising in the future. I was aware something was not right with my chewing – and I have not been pushing my recovery by eating foods I shouldn’t, at least from what I understood was OK. I occasionally like to gross sensitive people out by describing how it feels in detail. For example, it feels like my hard palate is a sheet of plywood, warping - though in my case, the axis of the warp has something to do with where the cuts were made, I think. Those who follow me who have had this procedure and are feeling this symptom, be warned! (Talk to your doctor!) Point is, I felt like it was not right, and I told everyone in sight – except my surgeon, the person who needed to know months ago. It did not occur to me that I should tell him; my understanding was, the recovery took a long time and I just had to be patient. That understanding did not serve me well. I don’t think it came from my surgeon, but I - a most motivated, curious, and frank patient – had that understanding nonetheless. Long-term Patient Health Advocacy side note: How much more would a patient who is timid, less-educated, or lacking strong support be hesitant to report important symptoms to a doctor who is not as responsive and open as mine? OK, it is what it is… I haven't been angry, and mostly not upset, though my life certainly has been upset. In less than three weeks I have a pair of major concerts I’m conducting with roughly 150 on stage and (hopefully) 600+ each night in the audience. (Skagit Valley Chorale, come see it!) I just started a new quarter at North Seattle College with a choir of 73 students and an online “Music in the United States” course as well. It’s not a great time to go into surgery. My surgeon and I discussed the circumstances at length, and he feels strongly that it’s important we address this as soon as possible – for my very long-term health. So, I’m making plans and hoping and praying for a quick recovery. Plans include careful eating, proper attention to medicines and recovery, care from others, colleagues helping, resting, and setting limits (in scheduling and in physical activity). I am concerned about how much I can handle, and how difficult the recovery will be. Last surgery, I was pushing limits a little to begin rehearsing 4 weeks after the surgery. This surgery will be MUCH less major, but I intend to rehearse 6 days after the surgery. How to balance the needs? What will be necessary? We’ll find out. (It’s in my mind that I should actually be preparing in other ways than writing this, but I want to get this down before the surgery. Perhaps less editing and re-writing this time. :) On the plus side, I have been able to see this as, "I get to go through the process again, knowing what I know now - and see what's different this time, what was helpful to have learned." I am (and Lorraine is) and expert on preparing the food I'll need, and feeding myself. I know how to deal with liquid medications and the syringe-catheter set up. I know that the second week will likely be the point when I get depressed. We've got lots of plans for how to handle it. Finally, “What is this surgery?” In brief: The mandible, chin, and nose surgeries are all healing well and require no additional surgery. In the surgery, the surgeon will remove the plates connecting my maxilla to my skull (sorry, anatomic shorthand, in haste). He’ll remove fibrous material that has grown, and implant (install?) a bone graft; a “cadaver ilium”. (Yes, I will have a dead person's hip in my hard palate. Um, part of it. Goes with the cadaver Achilles tendon in my knee.) Then he’ll install new plates slightly more forward/center of where they were, and sew me up. I’ll be in the hospital overnight, but should be able to go home next day. I’ll have several days at home, recovering. I will not need to be in the ICU after surgery as I was last time; my sleep apnea is no longer a factor in the surgery since the last repairs. Trumpet fanfare: Just found out recently that my AHI (Apnea-Hypopnea Index) has been reduced from 37 before the surgery (severe) to 16 now – much more manageable. Thank you, Surgery #1. I’ll hope to write again after the surgery. This time, I won’t have a lovely several weeks to write many times. (Wait, it wasn’t lovely last time…) …No, don’t want to end the post that way. How about a new song? In honor of my upcoming bone graft: Oh, the hip bone’s connected to the – jaw bone, now hear the word of the Surgeon. (Pardon the anatomical liberty – the maxilla is not a “jaw bone”… But the line scans better that way!)
1 Comment
In the search during my recovery for healthy and sustaining foods that could be eaten with little or no chewing, there was one area which had remained Off Limits. Oatmeal and all its brethren were not even a topic for discussion. More than three decades ago, far from civilization in the backwoods of British Columbia, I decided that I could not stand 7-grain cereal (in spite of not having other options for breakfast), and since then no hot cooked nasty mushy cereal has passed my lips. By contrast, Lorraine recently embraced oatmeal as part of her change in diet, and makes it nearly every day.
I did have a long and fairly healthy breakfast tradition of my own. Thankfully, even through the syringe-catheter diet and the no-chew diet, I was able to continue my decade-long love affair with a daily smoothie, now fortified with protein powder. (Whey, dude!) But, man cannot live by smoothies alone, and while I had always combined the smoothie with two homemade bran muffins in the past, that didn’t prove to be a good option in the post-surgery era. I attempted to eat a muffin several weeks ago, barely chewing – really just ‘gumming’ it – and trying to soften it in my mouth with milk (a messy affair). Because I couldn’t chew it, I had to break apart the crusty edges into very small bits that I could easily swallow with a minimum of gumming. I was watching the clock, so I know I do not exaggerate when I say that single muffin took 20 minutes of concentrated eating – and it was not an enjoyable experience. After that I abandoned the muffins (and most bready foods) and haven’t returned to them yet. I pieced together morning meals with other foods, though I always felt I was missing something central in my diet. However, a few weeks ago I was faced with a Saturday morning rehearsal followed by a board meeting. There wasn’t time to cook a serious breakfast, but I knew I needed to fortify myself well for the day with something beyond my smoothie. Somehow, the option that arose was a Quaker “Summer Berry” Oatmeal cup – just add water, stir, and wait for a few minutes. I made my bow to necessity, and accepted that I must eat this. While Lorraine drove, I ate (watching in the vanity mirror to make sure it went in my mouth). I ate it all, it fortified me, and I only gagged once! Undoubtedly a victory. Well, since that time I have – to my own surprise – embraced oatmeal as a regular, nay, a staple food. I’ve eaten several variations on the cup-of-oatmeal summer berry theme. (Umpqua, thumbs up! Fred Meyer Private Collection AWFUL – Where’s the berry?) I’ve made my own oatmeal several times (thick cut) and have learned that I can add all sorts of things to it, because, I must own, the texture still isn’t a great pleasure. So, lately I’ve been adding dried cherries, cranberries, strawberries, and blueberries – great sources of calories and fiber and other good stuff. (I add them early in the cooking process so they plump up nicely.) Just a little bit of brown sugar (Lorraine uses only vanilla, no sugar). I actually look forward to it. Who could have imagined such a turnaround? In fact, this experience and other food experiences through my recovery have caused me to think about exploration of mindfulness that my counselor has led me through. If much of our suffering is our own creation from the ‘stories’ we tell ourselves about what we’ve experienced, and if we can choose not to create our own suffering by letting go of such stories – then the story I’ve told myself for over thirty years about how I hate oatmeal, and how its texture disgusts me… could be just let go. Or, the stories I tell myself about foods I’ve never eaten – “I’m not going to like this, because it has a weird name,” or “I can tell by looking at this food that I’m not going to like it.” Or, other stories that cause me to suffer while eating or drinking: “I’m full but I have to eat a full serving even though I don’t want any more of this,” or “I haven’t drunk enough water today and now I’ve filled this glass full and I’m going to drink all of it now in one drink even though I feel like I can’t breathe because I have drunk so much in one go because I’m afraid if I don’t drink it all now I’ll forget later.” Just a few samples; all direct quotes I’ve had in my mind. As my counselor often asks me, when I’m holding tight to a thought that’s causing me pain, “Who would you be without that thought?” Lately, sometimes, I’m able to let those thoughts go, and surprise myself by liking the food that I knew I hated. Here we are at 5 Weeks + since my surgery! All indications are that recovery is going very well. And, I think it’s time to celebrate some victories in this process.
First, a win for something that didn’t happen: There have been no issues of VPI or hypernasality in my speech since the surgery. As you may recall from my pre-surgery posts, there was a concern that the advancement would stretch the pharyngeal flap and create conditions for VPI. My voice sounded pretty good even right after the surgery, but my surgeon cautioned us that congestion due to post-surgical swelling could obscure VPI. The swelling is now almost entirely gone, and still no VPI. I think we can call this a wonderful success. I have occasionally shuddered to imagine an alternate reality I could have experienced: struggling through that recovery while dealing with the trauma of realizing that my voice had reverted back to the nasality I began with as a small child, the self-consciousness of sounding like – as they labeled me then – a “crippled” person once again, and the knowledge I would have to go through therapy and possibly more surgery to correct it. Thankfully, this did NOT happen. And I must hand a great deal of the credit for that to my surgeon’s skill and care. Thank you, Doctor. Another victory is the fact that I’ve been able to re-assimilate into my musical work. I’ve had several rehearsals with Choral Arts Northwest, and will be singing the Duruflé Requiem this Sunday in concert. My singing voice is not 100%, but I can sing with decent tone and moderate power in the mid-range especially. In another victory, I’ve led three rehearsals with one of my choirs, the Skagit Valley Chorale. This group has well over one hundred singers this semester, and we have made an accommodation to help make sure I will be heard by everyone without straining: I am using a lavaliere microphone through a p.a. system. It is working very well. I think people can hear better than in rehearsals in the past – and I have been relieved at not having to worry about being heard. There is another victory whose possibility I have sensed, but not confirmed. With the advancement of my mandible and maxilla, it seems logical that both my pharynx and my mouth have greater volume. I have had the impression a few times when I have sung that I now have a larger resonating space for my voice – but I haven’t been able to really test this yet, for several reasons. My face is still numb and I don’t feel that I have good control over various muscles involved in singing, especially regarding changing vowels and changing formants. My hard palate area is still somewhat numb and doesn’t report reliable information about the sensations of resonation that I am used to. Also, I am not supposed to do vigorous activity, and full-power singing is a vigorous activity. I’ve found that the more power I put into my singing, the more it irritates the paresthesia in my face. I believe that the vigorous activity of singing can put pressure – similar to sneezing, straining, bearing down, and other activities I’m not supposed to do – on my healing facial bones that is not good for bone recovery, including the “bony union” at the advancement sites. As my surgeon releases me from limits on activity, and as my paresthesia begins to ebb, I’ll be able to explore this some more. I’m interested to see what my upcoming tests at the UW Speech and Hearing Clinic will show compared to the “before” tests we did in July. Anyway, I have a quiet and perhaps not-unfounded hope that I’ll find I have a richer tone than I did before the surgery. That would be exciting! The final victory that I’ll mention right now is just the recognition that my recovery continues to go well. One part of that victory is that I’m living with paresthesia day to day without freaking out about it. :) I trust it’s going to heal in time. Another is that I’m doing well at feeding myself, and not wasting much time being self-conscious or annoyed about realities like having to take lots of time preparing food, eating with a mirror and catching the dribbly bits that run down my chin, and drooling at any moment without knowing it (oh, joy). Friends, family, fellow musicians have been tremendously supportive, my spirits are good, and I seem to be handling the things I need to be doing, personally and professionally. May it continue so! Looking to the future… As you will have noticed, it’s been a while since I made a post. My music career – relatively quiet (hah!) during the summer – has picked up again with rehearsals and project management and study. One result of that is that I don’t have the same amount of time to write blog posts. Lorraine reminds me that if a blog is not updated on a regular basis, people stop checking it and readership goes way down. Yes, I know this to be true, and I accept it; I just don’t have the time to post regularly. The main impetus for this current spate of posts – my surgery and recovery – is winding down as my work winds up for the year. I’m certainly planning to make more posts – more about paresthesia, more about eating, and I’m sure other things like my upcoming work with speech therapy. But they will be fewer and farther in-between. So I’ll thank my readers who have gone on this journey with me, and say I’ll be back from time to time. Also, it has always been my intention that this blog will develop into many more areas of interest than my surgery and recovery. I look forward to finding out what’s going to inspire or prompt me to post! Yes, Mark Watney, the fictional hero of the book The Martian by Andy Weir, is a man who inspires me to be a better person. I wrote most of this post in my head two weeks ago, much earlier in my recovery, and just hadn’t gotten around to writing it out and posting it. But, tonight I finished listening to the audiobook and am inspired to give credit where credit is due: to author Andy Weir, to R.C. Bray, who read the audiobook, and to their creation, Mark Watney.
I’ve been listening to the book since my first day in the ICU after my surgery. In the first two weeks of my recovery, Mark Watney was my regular companion and helped me keep perspective. Thinking I had it bad? Mark had it much worse!
I admire Mark’s clever and creative mind, careful attention to details, knowledge in so many scientific fields, readiness and ability to work through the math, and perseverance in getting the tedious work done. His down-to-earth attitude and humor are also inspiring. Each time I listen to this book, I find myself trying to emulate these great qualities in my own life. What a wonderful thing, to be so moved by a work of fiction. Though I do like Disco. I’ve been studying about taste buds (at Wikipedia, that favorite source of true knowledge, and a few other sources) and have only just learned that the “taste bud map” concept, of zones on the tongue each responsible for one of the four different tastes, has been debunked. In fact, I learned that taste buds identify (at least) five different tastes: Salty, Sour, Sweet, Bitter, and Umami, a Japanese word meaning ‘savory’ – and those receptors are scattered not only on the tongue but all through the mouth.
I’ve found that I taste more when the food starts at the front of my mouth. I theorize, if you’re able to put food into your mouth with a utensil, you’re delivering it onto the tongue just behind the front teeth, and it has to travel past many taste buds on its way to the esophagus. On the other hand, if you’re getting food through a catheter, generally the food is delivered either to the back/middle of your mouth (if your teeth aren’t fastened shut) or at the far-back-right or -left side of your mouth (if your teeth are fastened shut and you’re running the catheter alongside the teeth). In those cases, the food passes by fewer taste buds – and in my case, it is skipping most of the taste buds that are ‘awake’ and reporting. This has interested me personally, as I realized recently that I am missing many flavors when I eat these days. As I had been trying to interpret my taste sensations according to the taste bud map, I wasn’t able to understand why I felt I was missing something along the hard palate and cheeks. Now that I understand better how taste buds work and are distributed, it has clarified why, when I gulp down a piece of Chef Boyardee “Mini Ravioli”*, and it glides along the roof of my mouth, I taste and feel almost nothing there. That’s just one example; much of the food I am able to eat via utensil travels that same path, and most of it has very little character. Now I understand: the areas in my mouth that are still numb, like the hard palate and the cheeks, are not able to report anything about taste and texture. I’ve been trying to think of a metaphor for how I’m experiencing this food – “… no more character than a lump of mud” or “… no more flavor than a lump of putty”, but have realized that nothing we eat is devoid of flavor and texture. I can’t describe my current experience of sensing no taste and no texture with a metaphor, because it’s unlike anything I have ever experienced. It is true that I can taste those ravioli on my tongue, so it’s not a completely flavorless experience, and I’m thankful for that. But it took me a while to understand why eating has so often been unrewarding. By missing some portion of the flavors and textures, I’m missing some of the built-in pleasure response to eating, which encourages us to eat as we need to. It’s not unusual lately that I have to require myself to eat, intellectually understanding it is necessary to take in food for the calories I need to sustain life and heal (and stave off depression). I sometimes am prompted to eat by hunger. But I am rarely prompted to eat by the anticipated pleasure of eating. This too shall pass, I am sure. More about Swallowing: I have recently come to understand more clearly the struggle I have been having with swallowing since the first day of recovery in the ICU. Having just read more about the amazing, complicated process of swallowing, I understand it better and can track at least some of the actions involved. Many times in this recovery when I’ve tried to swallow mucous or a last bit of food, I’ve felt that I couldn’t complete the swallowing process in the normal way. In particular, the muscles under the mandible (which I believe were stretched and shifted due to the genioplasty, poor things) feel numb and awkward when I swallow. I’ve theorized that some of these muscles that should be active in this process are numb and passive, and that those muscles that are working have to somehow make up for the others’ absence. However, when I asked my surgeon about this theory, he noted that the nerves involved in my surgery were sensory nerves, not motor nerves, and that my swallowing functions have not been impaired: this is just a sensation that I am having. Unfortunately, it seems that the sensations I’m having of some difficulty swallowing are leading me to try to “help” using muscles that have nothing to do with the process. I can often catch muscles in the back of my neck tensing up as I swallow. I’m not sure if that’s a primary reason why those neck muscles are much more rigid and tense than usual right now; I haven’t identified other behaviors yet that might be contributing. I’ll give my Alexander Technique training credit for helping me identify this unnecessary muscular work, but haven’t felt that I have been successful in using it to let go of those patterns very well. While I’m on the topic of the neck, I also realized recently that my front-of-neck muscles experienced their own trauma through the surgery and recovery. We could see yellowish areas on my neck for several days after the surgery – which I understand, perhaps imperfectly, were bruising related to the surgery. My surgeon said something to the effect that “gravity has an effect” on the bruising, and I gathered that it was ‘drifting down’ from the surgical sites and collecting in my neck. It seems my bruising was better than the norm, but it’s still something my neck has had to endure, along with continuing numbness under the jaw. I pet the muscles there every once in a while, but don’t have any idea how to encourage their healing. :) I’m conscious that I’m working too hard at swallowing whenever I’m aware of it. If I don’t have a completely “successful swallow”, I’m left with just a little remnant of the bolus (mostly mucous, I think), hovering in the pharynx, in a distracting and uncomfortable way. Perhaps this is a normal condition of life, and I have just made myself hypersensitive to it. On the other hand, I recall experiencing this sensation at many other times of my life, so it’s not just because of the surgery. Another mystery… Speaking of swallowing, and food that’s NOT helpful: I’ve tried a few wedges of Laughing Cow Cheese. This is very smooth processed cheese, meant to be a tasty treat. Instead, they are torture!, and I think my experience is something like that of a dog with peanut butter in its mouth. I theorize: when you can eat cheese with a cracker, the tongue uses the dryer bits of cracker as a tool to gather up the viscous cheese into a bolus that will hold together as it is pushed by the swallowing mechanism to the back of the throat and down. Crackers don’t work well with my no-chew diet, so I’ve just eaten the cheese alone, and hence the only material my tongue has had to work with is the cheese itself. Poor Tongue; it’s very frustrated! It can’t control the cheese, but unintentionally spreads it lavishly across the hard palate and into each nook and cranny of my teeth. It takes a lot of work to get the cheese headed in the right direction, to the esophagus – and once again, I feel my neck muscles getting tense as they work too hard, “helping”. Only 50 calories taken in, and I’m exhausted. Not worth it! Hmm, I might try preparing the cheese by crushing a cracker into bits and somehow combining them… Now, melted cheese of other kinds is great; it slides right down the gullet, no muss, no fuss, no struggle... *”Thank goodness for Chef Boyardee!” (I sing that to myself sometimes.) I continue to have numbness and paresthesia (a sensation of "pins and needles" varying from irritating to painful) in an area surrounding my nose, jaw, lips, and chin. Saturday (8/27) of last weekend I suffered from intense paresthesia, spent most of that day not doing anything but waiting to feel better, and then felt like I had wasted the day with no improvement to show for it. It wasn't until the next day that it dawned on me that I can't spend my days waiting for this to improve before living my life. After that I re-engaged a bit more in the activities of my life, and found that once I was not dwelling on it so much, the irritation and pain receded, somewhat, into the background.
I saw my surgeon a few days later, and commented that I had been trying to assess each day whether there had been any improvement in that pain. He cautioned me that day-to-day assessment is not appropriate for nerve regeneration, because this kind of healing takes much longer. Rather, we can assess on a monthly basis, or perhaps twice a month. He said, people who look for improvement in this area day to day just end up driving themselves crazy. Hearing this was a bit of a blow. Though it wasn't the first time he had told me of this, it was finally hitting home for me, and I realized that this is yet another challenge to be patient. Around that same time I had also been torturing myself with the fear that I might be among the small percentage of people who have permanent nerve damage, and that this condition will never improve for me. Statistics say that 85% of patients recover fully – but what about that other 15%? My counselor helped me consider this fear when we met last week. We reaffirmed my belief that I have an excellent surgeon who did a wonderful job in my surgery and who I trust when he tells me it's going to take a long time to heal. Also my counselor pointed out there are statistics about people having accidents while driving a car or flying in an airplane, and I don't spend time living in fear of those possible outcomes or let them stop me from driving or flying. If I answer his question, "Who would I be without that thought?" (without that fear), I realize I would be more relaxed, comfortable, and happy. So, I think I'll stay there, and I’m happy to say I have let go of that fear. I am thinking about ways of being pro-active, though -- just a bit. My surgeon OK'd light touching of my face, just saying "hello" to the soft tissues and stimulating the nerves, not disturbing the healing work of the bones, etc. I won't call it "massage" because that implies too much depth and pressure. But loving touch - from myself, from Lorraine, from my parents, from anyone who wants to! - is all good, I think. I can't say that the nerves feel "better" as a result of such touching: I think that looking for results like that takes me right back into the trap of trying to identify and gauge short-term improvements. But I feel better, and I trust that all those good vibrations and good energy are beneficial for me, even if I don't know how. Kind of like prayer, I suppose. I'm still finding material to write about regarding my experience in the hospital, and working it in as I have time. In this post I’ll address several sources of discomfort that I experienced while recovering in the ICU. It does seem to me that there is a host of people who have experienced all these discomforts and many worse ones – so who am I to write with any authority about this? What I do have is a growing passion that thoughtful and thorough information on any given medical issue be made available and actively presented to patients. I’ll hope to make my small contribution to the information and perspective available on the internet, encouraging potential patients to learn about what they are in for and ask questions of their surgeons, to help prepare as best they can.
To start, I’d like to follow up on a post I recently made in which I discussed some ways I've experienced feelings of suffocation in the past, and talk about how I drew on this experience as I was waking from my surgery. Once again I found myself struggling with similar feelings of suffocation and other problems with breathing, though now with a larger set of complicating factors. First, as I woke up the morning after my surgery I was acutely aware, intellectually if not tangibly, of the intubation that I knew had been threaded down my nose, through my vocal cords, and into my trachea to ensure the flow of oxygen through the surgery and initial recovery period. I had had conversations with my surgeon and anesthesiologist in which I expressed unease with intubation, specifically with the possibility of damage to my vocal cords. I understood that intubation was necessary and wasn't at all arguing against it; I was just expressing my concern to the professionals involved. I was appreciative that my anesthesiologist, hearing my concern about my voice, offered to use the smallest size tubing to help make less impact on the vocal cords. I believe that at least some of my unease came from 'anecdotal' information about damage to vocal cords (especially for singers), which I probably didn't understand fully and certainly couldn't tell you the source for, and also from a lack of knowledge about intubation itself. As a pro-active patient who usually informs himself very carefully, I am surprised now at the degree to which I remained ignorant and fearful on this topic. Looking into it now, I see that vocal cord damage is listed in reputable sources as a possible result of intubation. But though there is cause for caution, I have no information about how often it happens or the degree of damage, and it’s possible that if I had researched it more deeply before the surgery, I still would not have been able to gather enough information to feel more confident about that aspect of the procedure. I believe I did what I could in expressing my concern to the surgeon and anesthesiologist, that they responded to my concern, and that I’ve come out the other side with no apparent damage done. But, there in the recovery room, coming out of anesthesia, I remained frightened and uninformed. As I woke up in the ICU, I only became aware of myself and my parts gradually - so that, though I was awake at 7:30 a.m., I didn't realize I had a tongue until 9:30, became aware of the roof of my mouth a couple of hours later, sensed the length of my tongue a little later, and discovered the back of the pharynx later still. Like in those dental appointments of the past, I became aware of water, blood, or saliva that I felt I needed to do something with, but now didn't know what to do with it. I was afraid to try to swallow it because I knew that would force the vocal cords to try to close over the tube, since part of their function is to close off the trachea from anything being swallowed. It was only later that I learned of the balloon cuff near the end of an intubation tube which forms a seal preventing anything from getting into the trachea and the lungs (except the air flowing through the tube itself). At the time, I could feel the liquid rattle of something vibrating on my vocal cords – a deeply disturbing feeling, because I “knew” that meant I was in danger of breathing something liquid into my lungs. I couldn't cough it up and swallow it, and I couldn't do anything else about it either. Now, I understand that the cuff was preventing the liquid from entering my lungs – but I didn’t understand it then, and thought perhaps my breathing was compromised. I was able to write a note to the nurses about this fear, and they were able to set my mind at ease to some degree, though I still didn’t know about the balloon cuff. Also, when that liquid was present, the nurses would run another small tube into my other nostril and all the way down to the larynx (I think), where they could suction it out. My surgeon had carefully taught the ICU nurses how to do this when I came out of surgery (as Lorraine looked on), taking my pharyngeal flap into consideration and carefully maneuvering past it. I found that I could cooperate with this procedure by taking a very slow, careful, long breath and then coughing the liquid up, which helped collect it where it could be suctioned up more effectively. As time went on, I began to notice that different events made me fearful and likely to tense up. Using my Alexander Technique training, I often gave myself directions to release the tension as much as I was able, and even at times to inhibit the inclination to tense in the first place. - At some points while I was intubated, I felt like I was suffocating because I couldn’t breathe right. I had to settle myself down, think through it, and realize that the air was coming in through the tube, and that I had nothing to fear. I also had to inhibit any intention to phonate, and even had to inhibit a tendency towards curiously "checking" whether I could feel the tube anywhere. ("No, Adam, you really don't want to feel that.") - I had a blood pressure cuff on, which tightened to take my blood pressure every hour on the hour. I don't like the feeling of a tight cuff anytime, and in the circumstances (as I was somewhat out of it) I wondered if the pressure was cutting off the blood to my arm and even somehow interfering with blood flow in my whole body. - Both arms were restrained to the bed, as I had three IVs and the intubation, and it was important that I not inadvertently disturb any of them. Most of the time I was at peace with the restraints, but every once in a while I felt restrained and was disturbed about it. - Throughout the night (after I was extubated), while I was trying to sleep, it seemed that every time I felt myself starting to slide into sleep, a monitor beeped near my head. A nurse invariably appeared within a few seconds, checked the readouts, and turned off the alarm. I was thankful to be under such careful observation, but wished the darn alarm would stop going off just when I was finally starting to drift off. - My extubation (taking the intubation out) was a singularly unpleasant experience. I couldn't believe how long the tube was as the doctor drew it out of me. I don't know how you would prepare yourself for this. The (other) ICU doctor holding my hand comfortingly helped. It felt as if my soul was being pulled out of my stomach through my nose. (And Lorraine said it reminded her of the alien-coming-out-of-the-stomach scene in Alien.) Enough said. In many of these circumstances I was able to calm myself in short order. But each occasion that I experienced panic or fear was exhausting, physically and emotionally. I have wondered if it would have been helpful for me to have known more about what I was experiencing in advance. Something like "Your Guide to Staying in the ICU!". Maybe that exists on the internet - everything else does - but I haven't gone looking for it, and certainly hadn't before the surgery. Well, as with other posts I've written, perhaps reading this will prompt a patient to ask questions in advance, and learn a few answers to help him or her find a little more ease during the recovery. All this said, I would like to affirm again - and briefly discard anonymity - to say that the ICU staff at Overlake Hospital in Bellevue were tremendously helpful, competent, and caring for me when I was there. I've realized that though I wrote a very basic description of what was going to be done in my surgery, including the titles of the procedures - Maxillary Osteotomy, Mandibular Osteotomy, Genioplasty (Chin), Septoplasty & Inferior Turbinectomy (Nose) - there's a big difference between knowing the names and actually seeing what goes on. My family and I have watching some videos on YouTube that illustrate what was done to me.
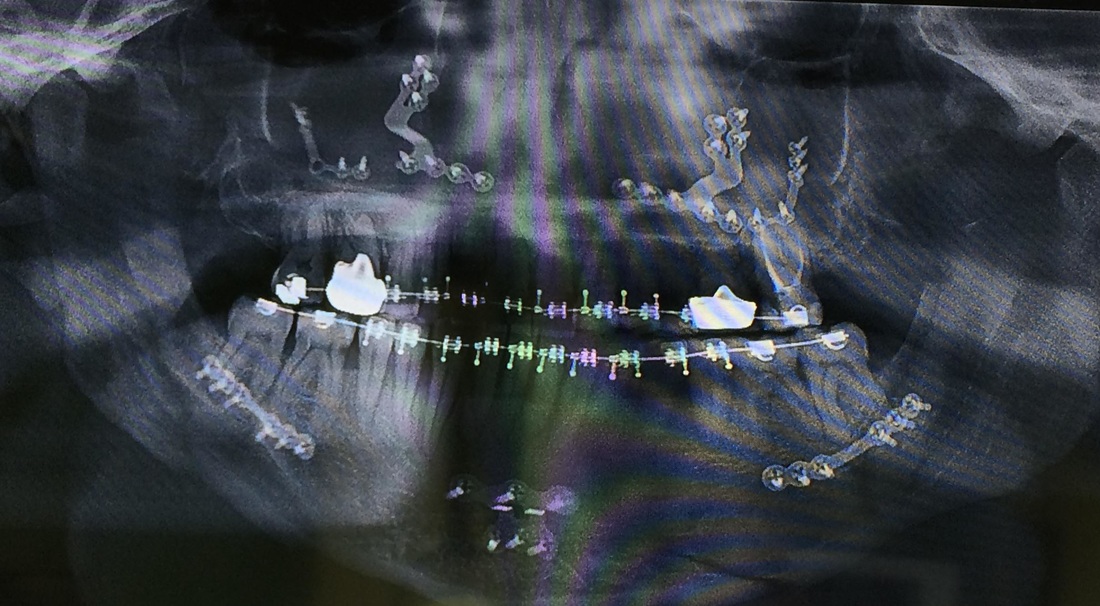
If you have the stomach for it - when they bring out the sawz-all and demonstrate cutting the mandible, that was just a bit much for me, even though it's just an animation - these are very interesting videos. Here's a video for prospective jaw surgery patients, showing the basics of what is done in different cases. In my case, the section from 3:58-5:00 shows what was done to me. Another short video showing roughly the same thing. At 1:30 the video shows something like my case, though in this example only the mandible (lower) is adjusted, while for me both the maxilla (upper) and mandible (lower) were advanced. Here's one addressed to surgeons in training, helping them learn the procedure. Shows more detail, though just in animation. Still not for the faint of heart! Now I'll also include a photo of an x-ray of me, post-surgery. In the photo, you can see my braces and a few crowns that replaced some molars. The rest of the hardware that shows up in the x-ray is titanium brackets and screws holding the advancement together. You can see they have been used for my mandible, maxilla, and chin as well. If you watch any of the videos, you can see demonstrations of hardware just like this being used. I look at those screws that are in my bones, and I think, "No wonder my face hurts!" I would feel remiss if the last thing I had to say about using a syringe and catheter was the struggle I wrote about in my first week of recovery - 10 days ago! So, in this post I’ll share a few things I learned that helped me manage the process of eating and medicating myself with the syringe-and-catheter set up. As always, I’m hopeful that any patient recovering from surgery like mine will find it helpful information. I’m going to address this blog post directly to those readers.
I’m thankful to Lorraine for her creativity, patience, and comfort in helping me through this aspect of my recovery. One of the hardest parts! I also want to give lots of credit for some basic foundational knowledge to Jonathan (JonPaul70 on YouTube), whose videos about eating with a syringe-catheter setup were fundamental and even inspirational. As Jonathan says, you don’t have to starve. There are many options for food out there that you can make work through a syringe. (And this man had to experience that for four+ teeth-wired-shut weeks, while I was cut free at 9 days…) I think Jonathan’s eating-demonstration and “don’t starve” videos cover most of what I would say here about food. Even though it’s not that important, I’ll include another tip from Jonathan just to make sure you get it: to keep the plunger moving easily in the syringe, coat the edges of its rubber stopper with olive oil. A big thank you to Jonathan -- You can see that thousands of people have watched his videos, and have probably been helped as I have. What I didn’t see Jonathan address in his videos was taking medications through the syringe, and this is the area that I struggled with the most. These are the medications and amounts I was taking: Sudafed (children’s) – 10 mil Oxycodone – 10 mil Durosill – 10 mil Amoxicillin – 10 mil Ibuprofen – 30 mil These varied in their noxiousness. The Amoxicillin wasn’t too bad for me, and neither was the Oxycodone. For the others, taking them in was never easy. Most mornings and evenings I had 4 medications to take at one time (keeping Oxycodone and Ibuprofen offset from one another). I always began with the ones that were the worst to take – Durosill and Ibuprofen especially. That way, it got easier as I worked through the list. Also, I would always alternate medicine and other drinks: 10 mil medicine, 60 mils good juice, 10 mils other medicine, 60 mils other comforting liquid, etc. That helped me calm down in between doses. For the first few days, I was squirting the medications undiluted straight to the back of my mouth and into my throat. I’m pretty sure they touched the “bitter” taste buds on the way, oh yes. Since I was bypassing my tongue (running the catheter along the side of the rubber-banded-shut teeth), it couldn’t help by performing its function of regulating the amount of liquid coming down. And, wanting to get it over with, I sometimes (often) squirted more in at a time than I should have. I sometimes kept the medicine coming, to “finish the dose”, when I wasn’t dealing well with what I already had in my throat, and really just needed to take a break for a few seconds. I found many times that 3 mil of medication – not a lot of liquid – was plenty to choke me if I wasn’t ready for it. At the worst times, the liquid coming in fast got down into my larynx and trachea and triggered a strong and painful cough, and I sprayed out medication on anything nearby. Miserable. Regularly a little bit of medication would get into my larynx, and depending on what it was, burn there. I was deeply concerned about some kind of damage to my vocal cords. I didn’t have any information about whether liquid medications sitting on the vocal cords can do damage, and I still don’t. I’ll hope to learn more about that in the future, but from an abstract (not experiential!) point of view. But in the meantime, it was certainly painful. If the first 3 mils of a 10-mil dose of Durosill (perhaps the worst of my medicines) were already causing me pain and discomfort, it was certainly hard pressing the plunger to deliver the remaining 7 mils. I’d usually deliver 3 mils at a time, very slowly, so 10 mils would take three or four times of gathering courage, taking the breath in, and gasping and lunging (can’t think of a better word) to take the medication in again. 30 mils of ibuprofen took an eternity, and I wasn’t displaying a lot of patience. Recipe for problems! And, sometimes the plunger wouldn’t move smoothly and would jerk forward accidentally, shooting in an extra several mils of medicine. That usually was upsetting and painful. (Reminder: OLIVE OIL on plunger helps keep it moving smoothly.) This remained the state of things through several cycles of medicine-taking in the first few days of my recovery. I had the intention of applying some Alexander Technique to the process, finding some means whereby I could better take in the medication in a controlled and thoughtful way. But I couldn’t rise above my response to the sensations and emotions aroused by the medications, and remained stuck in the patterns as described above. It wasn’t getting better or easier. Finally Lorraine realized that we could mix the medications with some other liquid (juice, smoothie) to make them easier to get down. (The food and medications are all mixed together down there in the stomach, after all - as long as they can be taken with food.) Once we thought of that, we started experimenting with different liquids to add. I found that a 3-1 mix, like 30 mils of something tasty with 10 mils of medication, seemed to dilute the Sudafed so that it wasn’t hard to take anymore. Docusill still wasn’t great even at a 5-1 mix, but it wasn’t painful anymore, just nasty. Ibuprofen didn’t benefit from mixing much, since at 30 mils there was only room in the 60-mil syringe for a 1-1 mix. Still, 60 mils of a somewhat less bitter mix was still somewhat better than 30 mils of straight Ibuprofen. I’m sure if I was still taking it I would have continued to experiment with different combinations, and perhaps I would have found something that more successfully masked it. Thankfully my run of Ibuprofen ended some time ago, so I didn’t have to keep at it. I encourage anyone trying out this “mixing” idea to experiment and try different things. I found that one of my favorite staples, Bolthouse Farms “Berry Boost”, helped mask the Sudafed (kids’ “grape” flavor, yum! Not). By contrast, apple juice combined with Docusill just made a much larger nasty drink, and likewise for a citrus-y drink combined with Ibuprofen. I settled on Bolthouse Farms “Stone Fruits” to combine with Ibuprofen, but it wasn’t great and I’d look farther afield now, if I still needed to. (I might never want to drink that flavor again, now.) You might be able to think ahead about what sorts of qualities the medicine has, and what sorts of qualities in the juice that might balance that well: for example, astringent mixed with creamy. Tip: When you combine the medicine and other drink, make sure you shake them up (carefully) together. In the photo you may be able to see that there are two purple colors in the syringe. One is the grape-flavored Sudafed, and the other is the Berry Boost smoothie – not mixed together, about 10 mils each this time. (Though it seems like the two liquids would combine when you draw in first one then the other into the syringe, it is an interesting function of hydrodynamics that they don’t, but stay separate, one liquid being sucked through the other.) If I had taken this as it was, I would have gotten a big surprise of several mils of straight medication, which would not have been pleasant. So, make sure to visually confirm that the medicine and the juice are mixed well. In the photo you’ll also notice I have a glass standing by of another drink. An innocuous Chocolate Protein Shake, a staple for me, is ready along with another syringe-catheter setup for when I’ve taken the medication and need to follow it with something comforting. Tip: For cleaning, vodka makes an excellent disinfectant. Somewhere Lorraine picked up a method to clean the syringe, plunger, and catheter: Mix a couple ounces of vodka with a cup+ of water. Draw in the vodka-water mix into the syringe, and squirt it out. Do this 2-3 times. Repeat with straight water 2-3 times. Done! (Vodka is also helpful when squirted into the armpits of smelly costumes, by the way.) At one point while struggling with all of this, I realized that I had not had any coaching on medicating with a syringe/catheter setup from any medical person. At first I was indignant at what seemed an oversight. But I realized that while I was in the ICU, I was on three IVs and constantly had medication and fluids coming in. So, there was no need to take any medications, and no opportunity to try taking additional medicine through a syringe-catheter. I’m not sure that a test run with something like water would have been to the purpose, as the issue with the medicine is dealing with its noxious qualities. And, with Lorraine’s help and as the staff looked on, I did a lot of eating via syringe on my last day, so they knew I was competent at that. I’m not sure what the answer is with this. I think more could be done to prepare patients before or just after surgery for this upcoming reality, but I’m not sure when. But, hopefully this posting will be a bit of help that is available – and might even prompt some improvements. Skip the part of taking the medicines straight! Go straight to mixing them! *** Note: I just realized that I could have split the 30 mils of Ibuprofen into three 10-mil servings, and made the proportions of whatever I mixed with it much higher. It never occurred to me, mostly I think because I always just wanted to get it over with. But I'll leave that thought here as another option... This post has been difficult to write, and has taken over a week. Much of it I wrote while my teeth were rubber-banded shut, which was a state that lent itself to feelings of suffocation. It has now been four days since my teeth were freed, and though I thought that freedom was going to feel like nirvana, I’ve since found that I’m still struggling with conditions that make me feel suffocated.
That’s actually a general theme for my recovery: there has been no dramatic turning point at which all became easy and relieved. (Hint to self: there isn’t going to be.) The same thing was true in my recovery from gall bladder surgery last year, and the same thing is true day to day in this process – and my memory is so short, I seem to have to re-learn patience every day. Then comes frustration that I’m not better at being patient. But sometimes I can see, thinking along lines my counselor has suggested, that such frustration is just a story I’m telling myself about this event in my life, an interpretation which is itself causing much of my suffering in this moment. Let go of the story, notice what is, and the frustration drops away – at least for now. Then I just do what I need to do, and get on with life. *** From last week *** I've been thinking a lot about suffocation - asphyxia - this past week. I've experienced a fair amount of what I would describe as mild suffocation during my recovery so far, with my teeth rubber-banded shut, my lips numb and sometimes resting in a closed position, and intermittent congestion in both nasal passages. My options are limited when these conditions are present, because I am not allowed to use pressure to blow my nose and clear the airway – if I even could successfully do that. There have been a few times when I have had to hold my mouth open with my fingers to keep a path for airflow. -- At this point I'll comment once again, thanks for Lorraine's combination of pragmatism and compassion! She came in the room to find me struggling to breathe as I re-enacted these conditions, and reminded me that I can run my CPAP, whose very purpose is to keep those airways open. OK, that's helping, and there's no reason to struggle for breath when I don't have to! -- Though the conditions are more extreme this week, some of them have been present for most of my life. The "septoplasty" procedure in my surgery was for the purpose of clearing away my deviated septum on the right side, which has partially blocked that airway for as long as I can remember. When combined with certain kinds of congestion, and a closed mouth, that blockage has often made me unable to breathe. I experienced that sort of suffocation several times in the period when dentists used rubber dams to isolate teeth for putting in fillings. That rubber dam also blocked off breathing from the mouth, and I was told to "breathe through your nose". Unfortunately, by that point in the procedure I usually couldn't point out that I wasn't able to breathe that way. (After a while I finally got proactive and asked them not to use the dam at the beginning of the appointment.) I spent a lot of time in circumstances like that controlling my breath and controlling panic as well, usually for the whole time until the dam was removed. Even when the rubber dam was not in use I had to learn how to manage breathing in dental and orthodontist appointments. I found that when I was partially congested, certain behaviors could worsen my congestion during the appointment. I learned that abrupt "snorting" breaths - the breaths I was likely to take when I felt suffocated and wanted a lot of air fast - would likely disturb the mucous in my nasal airway and create the very blockage I was trying to avoid. Only by taking in a controlled, slow-moving breath past the congestion could I keep the airway open. I often had to resist an impulse to panic at those times. I also had to remain calm when I had saliva or water in my throat that I was trying to keep from going down my windpipe. Sometimes I would be able to swallow the liquid, but other times I just had to manage it, keeping it isolated until someone noticed it and removed it with suction, while simultaneously maintaining that slow, steady breath to keep the congestion undisturbed and the airflow unimpeded. Through most of my considerable dental- and orthodontic-patient experience, I didn't discuss this with anyone. Only recently, as I worked several times with a very experienced and informative hygienist at my periodontist's office, had I begun to broach the topic. Unfortunately she has retired, but I am hopeful I can continue exploring the topic with others and learning some better strategies for coping successfully with this issue. *** Now, this week *** Though the CPAP was helpful in this recovery period for waking use, I’ve tried several times to return to using it for sleeping, but had to abort, usually after disturbing and uncomfortable sequences of suffocation, panic, and frustration. Last night (8/28) was my first success with the CPAP for sleeping since the surgery. I hadn’t intended to use it, but I was experiencing complete congestion in my nose, and as I tried to sleep with my mouth open, severe dryness was setting in immediately each time I tried to fall asleep. The CPAP mask confines my mouth and nose to only the air coming from the machine, and hydrates that air to help keep me from drying out as much. Things began roughly, as the severe congestion led to pretty much immediate feelings of suffocation when I put on the mask. But last night the fear grew greater than I had ever experienced before, into an unreasoned panic that the machine might actually stop, I’d be unaware or unable to rip off the mask, and that I would die of suffocation. It took a while to “talk myself off the ledge” and be able to accept surrendering my breath to a machine. Finally around 4:00 a.m. this morning I was calm and breathing regularly with the CPAP, and fell asleep. I’m still struggling with this panic that comes and overwhelms me when I can’t breathe. I don’t know if we all have this conditioned response, or if it’s more powerful in me. I don’t know how to make it better, and I don’t know how to not respond to the fear. It’s hard to trust that this is going to get better, and that I’m not going to feel starved for air for the rest of my life. My surgeon says it could be months. I’m looking forward to a day when my lips aren’t numb and can be a little more helpful (staying OPEN; how about that?!) so they don’t accidentally block my breathing. I’m looking forward to experiencing that freedom of air movement through my nose that I found just after waking up from surgery, before the swelling kicked in and blocked it. I’m looking forward to freedom from congestion in my nasal passages, so that I can take an easy breath through my nose just like they do in the decongestant commercials. And actually, I recognize that I do know something about making it better. I’m going to have to be more intentional about some things I do. Sometimes the conditions that cause my suffocation are brought about by my own impatience, like when I try to drink or eat just a little bit too much in this mouthful, even though I can feel my body wants breath right now, not food or drink. I can also help by revisiting my steps from the Alexander Technique – first asking for ease, which naturally lets me get out of the way and let my body breathe itself. |
AuthorDr. Adam Burdick has been a professional musician for over two decades. Teaching, conducting, and performing in various music genres, he is also a perpetual student with interest in a wide range of topics. He loves to ponder and share his discoveries with anyone interested! Archives
April 2017
Categories |

 RSS Feed
RSS Feed